Articles
Filter by Topic
- Adaptive Sport 1
- Artificial Intelligence 1
- Bike Labyrinth 3
- Bone density 1
- Brachial Plexus 2
- Bridging the Gap 1
- Bridging the Gap 1
- Carbonhand 4
- Cardiovascular 1
- Cauda Equina Syndrome 1
- Client Stories 4
- Cognition 1
- Company Updates 3
- Decision Making 2
- Dementia 1
- Denervation 27
- Diabetic Foot 12
- Efficiency 1
- Electrotherapy 32
- Exercise Benefits 33
- FES Cycling 20
- Fatigue 1
- Functional Electrical Stimulation (FES) 61
- Gait 2
- Goal Setting 5
- Grip 3
- Guidelines 1
- HRV 1
- Healthspan 2
- Indego 13
- Lifestyle 10
- Lower Motor Neuron 1
- Mobility 17
- Motivation 2
- NMES 3
- Nerve injury 2
- NexStride 1
- Occupational Therapy 1
- Orthotic 15
- PRAFO 29
- Pain 7
- Parkinsons 2
- Pressure Ulcers 16
- Product Updates 7
- RISE Stimulator 13
- Safety 2
- Spasticity 2
- Sponsor 1
- Standing 5
- Stim2Go 7
Article Length
- 1 minute read 3
- 10 minute read 21
- 11 minute read 4
- 12 minute read 10
- 15 minute read 13
- 18 minute read 1
- 2 minute read 4
- 24 minute read 1
- 25 minute read 1
- 26 minute read 1
- 28 minute read 1
- 3 minutes read 9
- 4 minute read 34
- 5 Minute read 16
- 6 minute read 6
- 7 minute read 17
- 8 minute read 9
- 9 minute read 3
- FES 2
- FoG 1
- Long Read 1
- PRAFO 1
- Seven Minute Read 1
- awareness 1
- carbonhand 2
- cognitive 1
- cues 1
- freezing gait 1
- freezing of gait 1
- gait 1
- neurological 1
- neuroplasticity 1
- nexstride 2
- occupational therapy 1
- occupational therapy day 1
- orthopaedics 1
- orthotic 1
- parkinson's 1
- pressure 1
- pressure relief 1
- prevention 1
- rehabilitation 2
- stroke 1
- ulcers 1
- world stroke day 1
Floating Heels: What the 2025 International Pressure Injury Guideline Means for the PRAFO
Heel pressure injuries are one of those problems where the evidence has been ahead of everyday practice for years. We have known for many years that pillows and improvised supports rarely keep a heel clear of the bed for long, and that a heel touching anything is a heel under pressure and shear. The 2025 International Pressure Injury Guideline (the fourth edition produced by NPIAP, EPUAP, and PPPIA) has now caught up to that reality, and in doing so it has changed the language clinicians and commissioners should use when they think about heel protection.
The guideline introduces a phrase worth noticing: "floating heels."
It is not a marketing line. It is a clinical description of what an effective heel offloading intervention has to achieve, taken from the guideline itself. And it has practical implications for any service that has to choose, fund, or audit heel protection equipment.
Our FES Cycling Reading List: Nine New Articles from fescycling.com
We have just recently redeveloped our sister site, fescycling.com, dedicated to functional electrical stimulation cycling: the evidence, the practicalities, and the questions that come up most often in clinic. The articles below are written for people considering FES cycling, the families and case managers supporting them, and clinicians who want a clearer view of what the technology can and cannot do.
If you are new to FES cycling, the first three are the natural starting point. The rest go deeper into specific questions, conditions, and day-to-day reality. Although our offered system is based on the Stim2Go unit from Pajunk, the articles should be of general interest to those who wish to learn more about FES cycling.
If you'd like more, there is a comprehensive online resource available at https://fescycling.com/guide and a AI powered chat to let you explore it.
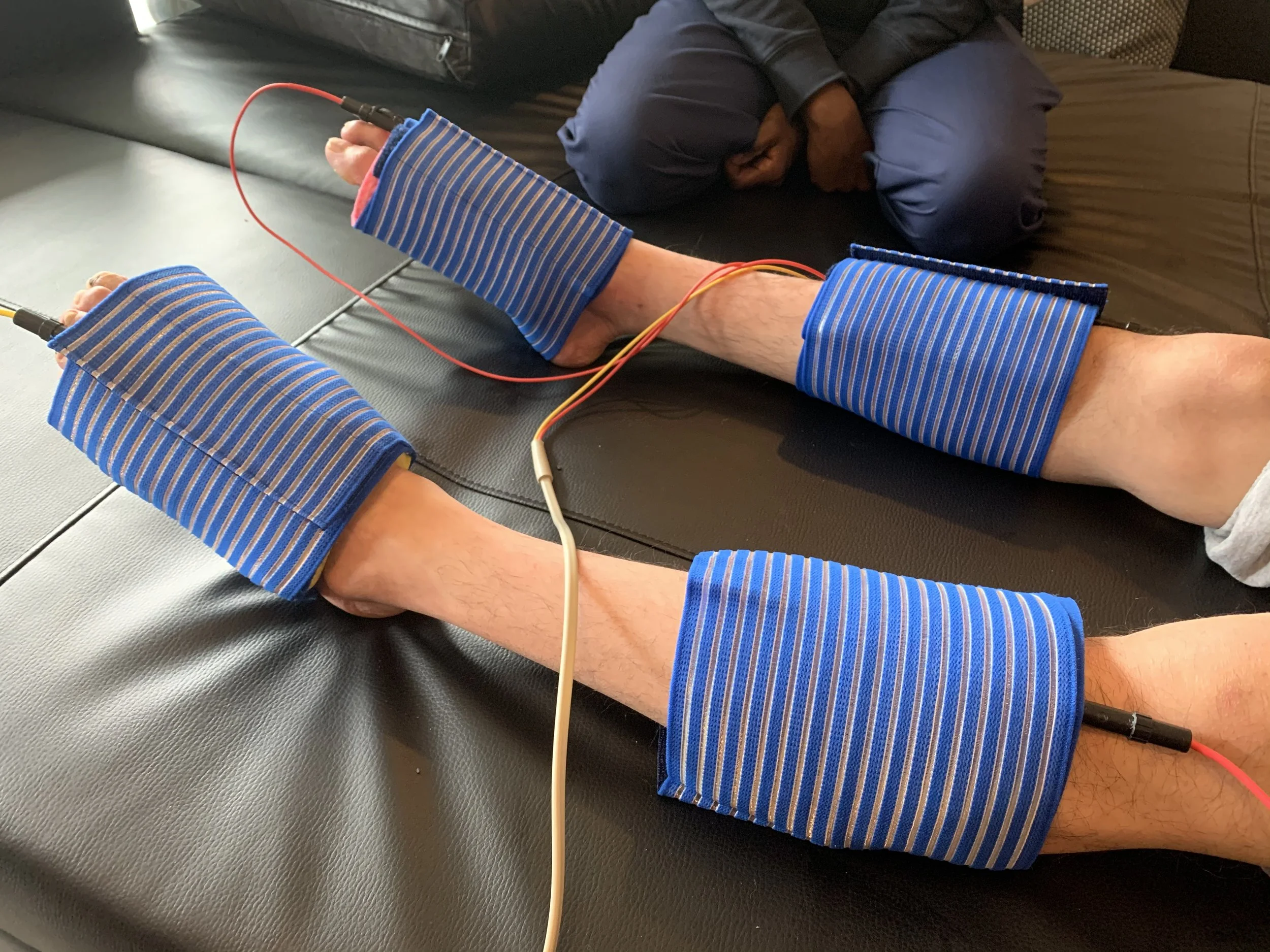
Normal vs Denervated Muscle: Why the Rules of Electrical Stimulation Change After Nerve Injury
It is quite common for us to meet clients who have tried electrical stimulation on a limb and found that nothing happened. No matter how high the intensity was set, the muscle simply would not contract. They arrive frustrated, sometimes having been told that nothing more can be done. When we then use the RISE Stimulator, a specialist device capable of producing the long-impulse-duration waveforms that denervated muscle actually requires, they are often surprised and relieved to see a contraction for the first time.
That moment of surprise reveals an important gap in understanding. The muscle did not fail to respond because it was beyond help. It failed because the wrong electrical 'language' was being spoken. A denervated muscle is not simply a weak muscle. It is, in a very real sense, a different tissue with altered structure, electrical properties, and activation rules. Understanding these differences is the foundation for making sense of any treatment approach.
Transcutaneous Vagus Nerve Stimulation and Transcutaneous Spinal Cord Stimulation - Parallels for Rehabilitation Practice
Two non-invasive neuromodulation technologies — transcutaneous vagus nerve stimulation (tVNS) and transcutaneous spinal cord stimulation (tSCS) — are reshaping how we think about neurological rehabilitation.
Although they target different levels of the nervous system, these modalities share a surprising number of fundamental principles. Understanding these parallels gives clinicians, patients, and carers a clearer picture of how modern neuromodulation works, what to expect from treatment, and why these technologies represent a genuine shift from compensatory to restorative rehabilitation.
This article identifies ten fundamental parallels between tVNS and tSCS, drawing on the published scientific evidence to explore what they have in common, where they differ, and what this means for clinical practice.
Electrical Stimulation After Nerve Repair Surgery: When to Start and What to Expect
Nerve repair surgery—whether nerve grafting, nerve transfer, or direct repair—offers hope for people with peripheral nerve injuries, including brachial plexus injuries. However, surgery is just the beginning of the recovery journey. After the surgeon has reconnected or rerouted nerves, there's a waiting period while regenerating nerve fibres grow toward their target muscles. This process is slow, measured in months rather than weeks.
During this waiting period, a critical question arises: what happens to the muscles? Without nerve signals, they begin to atrophy and deteriorate. If the muscle degenerates too severely before reinnervation occurs, even successful nerve regeneration may not restore function—the nerve reconnects, but finds a muscle no longer capable of responding.
This is where electrical stimulation plays a crucial role. By keeping muscles viable during the reinnervation window, stimulation can significantly improve the chances of functional recovery. In this article, I'll explain how nerve regeneration works, when to consider electrical stimulation, and what to expect throughout the process.
Why structure beats willpower in neurological rehabilitation
If motivation were enough, rehabilitation adherence (sticking to the effort of training to recover) would not decline so predictably. But it does. Across conditions, across populations, the pattern is the same: strong engagement in the early weeks, followed by a steady fade. Not because people stop wanting to recover — but because motivation, by its nature, is temporary. It is a mood, not a method.
After decades of working in this field, I can tell you that the people who sustain their efforts over months and years are rarely the most motivated. They are the most structured. They have built something that works regardless of how they feel on any given morning — when they are tired, in pain, frustrated by slow progress, and wondering whether any of this is actually working.
To achieve significant functional gains and take advantage of neuroplasticity, it takes sustained, high-quality repetitions. Without structure, success will be elusive.