Articles
Filter by Topic
- Adaptive Sport 1
- Artificial Intelligence 1
- Bike Labyrinth 3
- Bone density 1
- Brachial Plexus 2
- Bridging the Gap 1
- Bridging the Gap 1
- Carbonhand 4
- Cardiovascular 1
- Cauda Equina Syndrome 1
- Client Stories 4
- Cognition 1
- Company Updates 3
- Decision Making 2
- Dementia 1
- Denervation 27
- Diabetic Foot 12
- Efficiency 1
- Electrotherapy 32
- Exercise Benefits 33
- FES Cycling 21
- Fatigue 1
- Functional Electrical Stimulation (FES) 62
- Gait 2
- Goal Setting 5
- Grip 3
- Guidelines 1
- HRV 1
- Healthspan 2
- Indego 13
- Lifestyle 10
- Lower Motor Neuron 1
- Mobility 17
- Motivation 2
- NMES 3
- Nerve injury 2
- NexStride 1
- Occupational Therapy 1
- Orthotic 15
- PRAFO 29
- Pain 7
- Parkinsons 2
- Pressure Ulcers 16
- Product Updates 7
- RISE Stimulator 13
- Safety 2
- Spasticity 2
- Sponsor 1
- Standing 5
- Stim2Go 7
Article Length
- 1 minute read 3
- 10 minute read 21
- 11 minute read 4
- 12 minute read 10
- 15 minute read 13
- 18 minute read 1
- 2 minute read 4
- 24 minute read 1
- 25 minute read 1
- 26 minute read 1
- 28 minute read 1
- 3 minutes read 9
- 4 minute read 34
- 5 Minute read 16
- 6 minute read 6
- 7 minute read 17
- 8 minute read 10
- 9 minute read 3
- FES 2
- FoG 1
- Long Read 1
- PRAFO 1
- Seven Minute Read 1
- awareness 1
- carbonhand 2
- cognitive 1
- cues 1
- freezing gait 1
- freezing of gait 1
- gait 1
- neurological 1
- neuroplasticity 1
- nexstride 2
- occupational therapy 1
- occupational therapy day 1
- orthopaedics 1
- orthotic 1
- parkinson's 1
- pressure 1
- pressure relief 1
- prevention 1
- rehabilitation 2
- stroke 1
- ulcers 1
- world stroke day 1
Why structure beats willpower in neurological rehabilitation
If motivation were enough, rehabilitation adherence (sticking to the effort of training to recover) would not decline so predictably. But it does. Across conditions, across populations, the pattern is the same: strong engagement in the early weeks, followed by a steady fade. Not because people stop wanting to recover — but because motivation, by its nature, is temporary. It is a mood, not a method.
After decades of working in this field, I can tell you that the people who sustain their efforts over months and years are rarely the most motivated. They are the most structured. They have built something that works regardless of how they feel on any given morning — when they are tired, in pain, frustrated by slow progress, and wondering whether any of this is actually working.
To achieve significant functional gains and take advantage of neuroplasticity, it takes sustained, high-quality repetitions. Without structure, success will be elusive.
Is the Autonomic Nervous System Ever Truly "In Balance"?
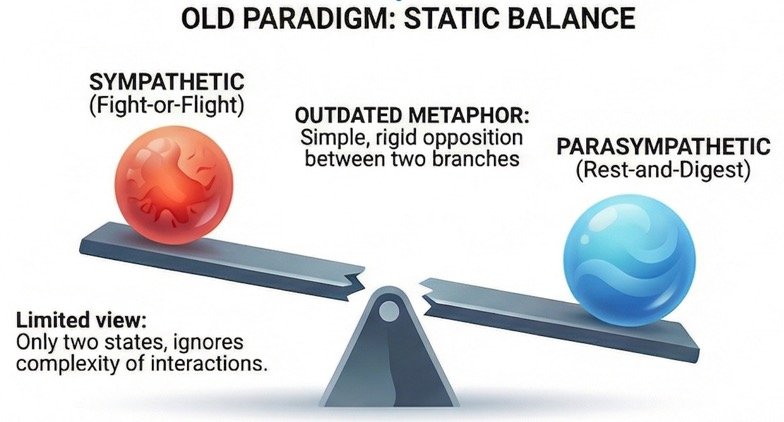
If you have been reading about the autonomic nervous system — perhaps because you live with a spinal cord injury, or you work with people who do — you will almost certainly have encountered the idea of "autonomic balance." The image is seductive: sympathetic on one side, parasympathetic on the other, and health is achieved when the two sit neatly level, like a set of scales in equilibrium.
It is a useful teaching shorthand. It is also, as modern physiology has demonstrated over the past three decades, an oversimplification that can actually mislead both clinicians and patients.
The fundamental question is this: does the autonomic nervous system ever truly achieve "balance" — and if not, what should we be aiming for instead? The answer has direct implications for how we think about autonomic dysfunction after spinal cord injury and for emerging interventions such as transcutaneous vagus nerve stimulation (tVNS) that aim to improve autonomic regulation.
Can I Start Electrical Stimulation Years After My Denervation Injury? What the Research Shows
One of the most common questions I receive comes from people who've had a denervating injury—whether spinal cord injury, brachial plexus injury, or another peripheral nerve condition—years or even decades ago. They've recently learned that electrical stimulation might help preserve or improve their muscle condition, and they want to know: Is it too late for me?
This is an important question that deserves a thorough answer. The research evidence and my clinical experience both suggest that while earlier is definitely better, "too late" is rarely the correct conclusion. In this article, I'll examine what the evidence actually shows about late intervention, which factors influence outcomes, and how to decide whether it's worth trying in your specific situation.
We don't discuss the technical aspects of stimulation. This has been covered in other articles on this site. Recognise, however, that the stimulation patterns are designed to work directly with the muscle fibre and do not rely on an intact peripheral nerve.
Spasticity After Spinal Cord Injury: When Medication Isn't the Answer
Spasticity is common after spinal cord injury, and while medication can help, it isn’t always the best or only option. This article explores alternative ways to manage spasticity when medication isn’t effective or suitable. It looks at why symptoms can vary, what triggers may make spasticity worse, and the importance of an individualised approach. From rehabilitation strategies to practical day-to-day management, it provides a helpful overview for improving comfort, function, and quality of life.
How Muscle Fibre Composition Impacts Electrical Stimulation Effectiveness
Electrical stimulation is a popular and widely used approach for physical rehabilitation. When used for muscle strengthening, it is necessary to take into account the fact that electrical stimulation produces muscle contractions in a relatively inefficient way.
In this article, we take a brief look at muscle fibre types. Following a neurological insult, muscle fibre types undergo transformation, producing changes that affect the ability of muscles to do work. We examine the particular case of spinal cord injury and consider how this affects the effectiveness of electrical stimulation.
Approaches to combat fatigue are examined. Finally, we consider attempts being made to improve the performance of stimulators and produce consistent muscle contractions under all circumstances.
Exploring Electrical Stimulation for Pain Relief
Neuropathic pain is a complex and debilitating condition that affects millions worldwide, disrupting daily life with sensations that defy typical pain narratives. For those living with chronic discomfort, the challenges often feel insurmountable. However, with an estimated 7–10% of the global population impacted, the demand for solutions has never been greater.
This article explores an exciting frontier in treatment—electrical stimulation. By directly engaging the nervous system, this innovative approach offers the possibility of relief where traditional methods have fallen short. What makes neuropathic pain so difficult to treat? And could electrical stimulation hold the key to improving quality of life for countless individuals?
Join us as we examine this cutting-edge therapy and its potential to reshape the future of pain management.