Articles
Filter by Topic
- Adaptive Sport 1
- Artificial Intelligence 1
- Bike Labyrinth 3
- Bone density 1
- Brachial Plexus 2
- Bridging the Gap 1
- Bridging the Gap 1
- Carbonhand 4
- Cardiovascular 1
- Cauda Equina Syndrome 1
- Client Stories 4
- Cognition 1
- Company Updates 3
- Decision Making 2
- Dementia 1
- Denervation 27
- Diabetic Foot 12
- Efficiency 1
- Electrotherapy 32
- Exercise Benefits 33
- FES Cycling 20
- Fatigue 1
- Functional Electrical Stimulation (FES) 61
- Gait 2
- Goal Setting 5
- Grip 3
- Guidelines 1
- HRV 1
- Healthspan 2
- Indego 13
- Lifestyle 10
- Lower Motor Neuron 1
- Mobility 17
- Motivation 2
- NMES 3
- Nerve injury 2
- NexStride 1
- Occupational Therapy 1
- Orthotic 15
- PRAFO 29
- Pain 7
- Parkinsons 2
- Pressure Ulcers 16
- Product Updates 7
- RISE Stimulator 13
- Safety 2
- Spasticity 2
- Sponsor 1
- Standing 5
- Stim2Go 7
Article Length
- 1 minute read 3
- 10 minute read 21
- 11 minute read 4
- 12 minute read 10
- 15 minute read 13
- 18 minute read 1
- 2 minute read 4
- 24 minute read 1
- 25 minute read 1
- 26 minute read 1
- 28 minute read 1
- 3 minutes read 9
- 4 minute read 34
- 5 Minute read 16
- 6 minute read 6
- 7 minute read 17
- 8 minute read 9
- 9 minute read 3
- FES 2
- FoG 1
- Long Read 1
- PRAFO 1
- Seven Minute Read 1
- awareness 1
- carbonhand 2
- cognitive 1
- cues 1
- freezing gait 1
- freezing of gait 1
- gait 1
- neurological 1
- neuroplasticity 1
- nexstride 2
- occupational therapy 1
- occupational therapy day 1
- orthopaedics 1
- orthotic 1
- parkinson's 1
- pressure 1
- pressure relief 1
- prevention 1
- rehabilitation 2
- stroke 1
- ulcers 1
- world stroke day 1
Cauda Equina Syndrome and Denervated Muscle: Your Options for Long-Term Health
Cauda equina syndrome (CES) is one of the most challenging situations in spinal cord injury rehabilitation. Unlike injuries higher in the spine, CES directly damages the lower motor neurons—the nerve cells that connect to and control the leg muscles. This results in the muscles becoming denervated, losing their nerve supply completely.
For many years, people with CES were told little could be done about the muscle wasting that occurs. The common belief was that denervated muscles would inevitably weaken, and electrical stimulation—which is effective for higher spinal injuries—simply wouldn't help. That perspective has shifted.
Research over the past twenty years shows that denervated muscles can be preserved and even improved with appropriate electrical stimulation—however, it requires a different approach from standard rehabilitation methods. In this article, I will explain what happens to muscles after cauda equina syndrome, why conventional methods often fail, and what options are available for maintaining long-term muscle and tissue health.
Why Pillows Fail: The Biomechanics of Heel Suspension
The pillow remains perhaps the most commonly used heel elevation method in hospitals worldwide. I guess this is because they are readily available, cost nothing beyond what's already supplied for patient comfort, and require no special equipment or training. They are also inadequate for heel protection and can compromise continuity of care.
The evidence is now clear: an Australian multi-centre ICU trial found that purpose-designed heel offloading devices achieved a 0.4% pressure injury incidence, compared to 8.4% with standard care, which typically means pillows and repositioning [1]. That's a twenty-fold difference. Translated into practical terms: for every 1,000 patients, 79 fewer will develop heel pressure injuries when proper offloading devices are used instead of pillows.
This isn't a criticism of clinical staff who use pillows—they're working with what's available and following long-established practice. It's an observation about biomechanics: what a pillow can and cannot achieve when the goal is heel offloading.
Understanding why pillows often fail points toward what effective heel protection actually requires.
Is the Autonomic Nervous System Ever Truly "In Balance"?
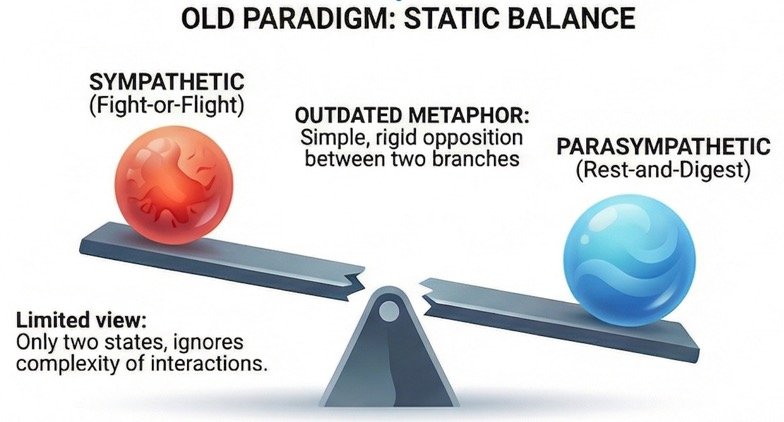
If you have been reading about the autonomic nervous system — perhaps because you live with a spinal cord injury, or you work with people who do — you will almost certainly have encountered the idea of "autonomic balance." The image is seductive: sympathetic on one side, parasympathetic on the other, and health is achieved when the two sit neatly level, like a set of scales in equilibrium.
It is a useful teaching shorthand. It is also, as modern physiology has demonstrated over the past three decades, an oversimplification that can actually mislead both clinicians and patients.
The fundamental question is this: does the autonomic nervous system ever truly achieve "balance" — and if not, what should we be aiming for instead? The answer has direct implications for how we think about autonomic dysfunction after spinal cord injury and for emerging interventions such as transcutaneous vagus nerve stimulation (tVNS) that aim to improve autonomic regulation.
How to Choose a Stimulator for Denervated Muscle: What Actually Matters
If you've determined that you need electrical stimulation for denervated muscles, the next question is obvious: which device should you choose? This is where many people become confused — and understandably so. The market is flooded with electrical stimulation devices, most of which cannot help denervated muscles, and the technical specifications can be bewildering even for clinicians, let alone someone navigating this for the first time after a life-changing injury.
In my experience, the confusion isn't really about the number of options. It's about how devices that look similar on the outside — a box, some wires, a pair of electrodes — can be fundamentally different on the inside. A TENS unit from a pharmacy or bought online, and a specialised denervated muscle stimulator may appear related, but they are designed for entirely different physiological purposes. Choosing the wrong one isn't just a waste of money; it means lost time during a period when early intervention matters most.
In this article, I'll explain what features actually matter for denervated muscle stimulation, why most devices on the market are unsuitable, and how to evaluate your options
Transcutaneous Vagus Nerve Stimulation: An Approved Medical Device with Emerging Rehabilitation Promise
This article focuses partly on a specific device: the tVNS® system, manufactured by tVNS Technologies GmbH in Germany. This is not a wellness gadget or an unregulated consumer product. The tVNS device is approved as a Class IIa medical device under the EU Medical Device Regulation (EU-MDR) with CE marking—currently the only non-invasive VNS device with this level of EU-MDR approval. It is registered for four specific clinical indications: epilepsy, depression, chronic migraines, and Prader-Willi syndrome. Anatomical Concepts (UK) is delighted to distribute and support the tVNS® system in the UK.
Why does this matter for rehabilitation? Because the same mechanisms that make vagus nerve stimulation effective for these approved conditions—neuroplasticity enhancement and anti-inflammatory action—are precisely the mechanisms that show promise for neurological rehabilitation. The ongoing research into stroke recovery, spinal cord injury, multiple sclerosis, and other conditions builds on a foundation of established science and regulatory-grade engineering.
Shear Forces at the Heel: The Hidden Damage Mechanism
When clinicians think about pressure ulcer prevention, they typically focus on pressure—the perpendicular force that compresses tissue against a surface. This is understandable. The condition is called a pressure ulcer. Pressure is in the name.
But pressure tells only part of the story. Shear—the force acting parallel to the support surface that distorts tissue layers relative to each other—may be even more damaging than pressure alone. Research dating back to Bennett's seminal 1979 study demonstrated that when shear is present, the pressure required to produce vascular occlusion is reduced by approximately 50%. At shear levels of roughly 100 g/cm², the pressure needed to stop blood flow was half that required when little shear was present.
This finding has profound implications for heel protection. A device that reduces pressure but doesn't address shear may leave the heel vulnerable to the very damage it was meant to prevent.